Knowing Your Device and
Understanding Surgery
Over the years, advanced technology has been used to develop devices to help patients diagnosed with heart failure. Many of these devices, although designed for adults, have been adapted for use in children. Let’s explore each device and what to expect before, during, and after surgery.
Over the years, advanced technology has been used to develop devices to help patients diagnosed
with heart failure. Many of these devices, although designed for adults, have been adapted for use
in children. Let’s explore each device and what to expect before, during, and after surgery.
1
Pacemaker/ICD
2
VADs
3
Pre-Transplant
4
CardioMEMS™
Overview
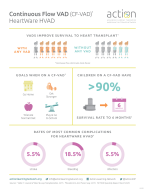
HVAD™ System
Notice to all Patients, Families, & Care Givers
Medtronic has stopped the distribution and sale of the HVAD™ System as of June 3, 2021(see full press release). Children and young adults who are currently supported with an HVAD™ System will receive the same excellent care from their care teams. Our ACTION education material is still relevant for those supported by the HVAD™ System. Contact your care team with any questions.
Overview
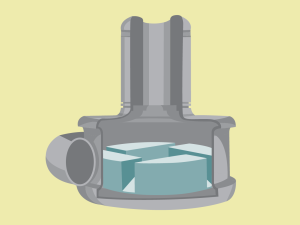
The HVAD™ System will work by continuously spinning blood from the weak part of the heart, through the device, out to the aorta, and the rest of the body. There is a small impeller located inside the VAD that helps with this spinning motion. The pump is always connected to a controller and a power source that keeps the VAD spinning. Because the continuous flow device bypasses the weakened heart chamber, you may not be able to feel your pulse.
Want more information? See our HVAD™ System ACTION Patent Education Handbook.
While VADs have been shown to help many patients, living with a VAD has its challenges. VAD patients must:
- take blood thinners and other medicines to help the heart
- make frequent visits to the doctor to make sure the VAD is working right
- have a 24-hour caregiver who understands how the pump works
- change the bandages and clean the area where parts of the pump meet the skin
Learning about your VAD is an important part of getting you discharged and keeping you safe. Watch this video to learn more about how your device works:
Your care team will provide you with more in-depth training to prepare for the VAD quiz that you and your caregivers must complete before leaving the hospital.
-
Device Components
-
Benefits
-
Risks
Device Components
The equipment is life-saving and managing it may feel overwhelming. However, learning how each of the pieces work together will help you feel more comfortable in your daily journey.

1 HVAD
The HVAD is implanted inside of your chest. The outflow graft is a flexible tube that connects the outflow of the pump to the aorta. It helps carry the blood from the pump to the rest of the body. The inside of the pump has an impeller that spins continuously and can distribute up to 10 liters of blood per minute (L/min).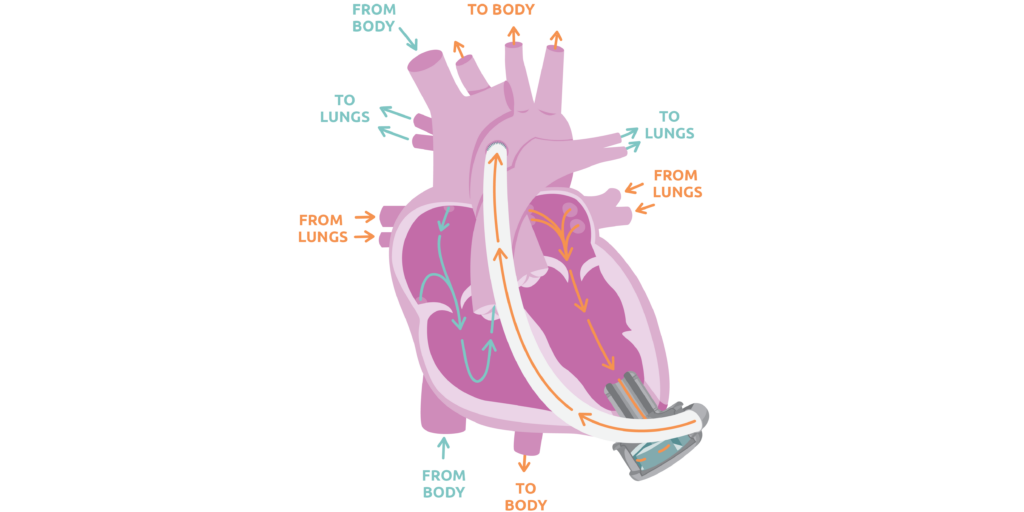
2 Driveline
The driveline cord is filled with electrical wires that connect the HVAD to the controller (the brains of the HVAD). This cord performs two functions to help the device work properly. The HVAD (inside the heart) transfers important information to the controller through the driveline. The driveline also brings power back to the pump to make the HVAD spin. Never disconnect your driveline because this would make your pump stop.
3 Monitor
You will only be plugged into the monitor when you are in the hospital or in a clinic. The monitor tells your care team how your device is working so they can make any adjustments needed.
4 Controller
There is a port where the driveline enters the controller and transfers power and information. The controller provides power to the pump, and the pump sends vital information back about how the pump is working.

Pump Parameters
There are many numbers that you will want to know about. The RPM, or rotations per minute, is set by your care team. The other numbers are calculated but will tell the team a lot about how you are doing.

Download PDF
To learn more about alarms and troubleshooting, reference your ACTION HVAD™ System Patient Education Handbook, or the HeartWare™ HVAD™ System Patient Manual given to you on or before your surgery or watch the Learning Alarms & Troubleshooting interactive below.
Electrical Power
You must avoid being away from electricity for a long period of time.
- Wall Charger: The AC adapter connects from the wall to the controller. When using the AC adapter, the controller only pulls power from the wall. However, a battery should always stay connected to the controller when using an AC adapter.
- Batteries: A single battery can last 4–7 hours. When the controller is connected to 2 batteries, it drains one battery at a time providing a maximum of 12 hours.
- Battery Charger: The battery charger dock is a charging station for the batteries.
Benefits

A HVAD™ System can be used to help a heart pump for many reasons. Depending on your situation, it may be used as:
- Bridge to Transplant: To support the heart until the best donor heart is available for transplant.
- Destination or Chronic Therapy: To support the heart, decrease heart failure symptoms and improve overall quality of life.
- Bridge to Recovery: To support the heart if there is a chance the heart will recover.
- Bridge to Decision: To support the heart until a decision can be made by the family and medical team regarding next steps (surgeries or medications).
A HVAD™ System may help reduce heart failure symptoms and improve quality of life as you continue along your journey.
Is this VAD Right for Me?
Find out if a continuous flow HVAD™ System is right for you.
Risks

There are also some risks associated with having a VAD, but your care team will work hard to keep you safe.
Infection
The driveline comes out of your belly and will need to be cleaned frequently. This is important because bacteria lives on your skin and may cause an infection at your driveline site. You may feel nervous the first few times your dressings are changed, but your care team will be there to support you.
Stroke
There is a risk of stroke with all VADs. A clot can form in the VAD, become dislodged, and may travel up a blood vessel to the brain. A blood clot in the brain leads to a decreased blood flow to the brain in that specific area, and this is called a stroke. Your care team will manage your blood thinner medicines and levels carefully to try to prevent a stroke. Sometimes, even with perfect levels, a stroke will occur.
Your care team will monitor you for the following symptoms:
- Headache
- Confusion
- Numbness and/or tingling on one side of the body
- Weakness on one side of the body
- Slurred speech
Bleeding
There is a risk of bleeding with all VADs. To prevent clots from forming in the device, you have to be on a blood thinner. Sometimes the blood thinner will lead to bleeding that may require a change in medicines, a blood transfusion, or in some cases, a surgery to stop the bleeding. Your care team will manage your blood thinner medicine and levels carefully to try to prevent bleeding. Sometimes, even with perfect levels bleeding will occur.
Pediatric VAD Infections
Download the pdf to learn more.
Take ACTION Reducing Stroke Rates
Download the pdf to learn more.
Device Components
Cannulae
During VAD surgery, your heart surgeon will place cannulae that are special tubes made of a very soft silicone material. These soft cannulae will come out of your lower chest area just below your breastbone.
Your heart has two pumping chambers, a left ventricle and a right ventricle. Your cardiologist and surgeon will decide if you need support on just one ventricle or both. If you only need support for one ventricle, you will have two cannulae. If you need support for both ventricles, you will need four cannulae.
Blood Pump
The soft cannulae connect to a blood pump that is chosen especially for you. This blood pump is hand-crafted by scientists and engineers to provide adequate blood flow to your entire body. It’s like a little heart that is outside of your body.
Your blood pump has another tube connected to it where air will move in and out of it. But don’t worry, the air will not go into your body. Instead the air helps the blood pump to fill and push blood out just like a real heart can.
IKUS
The IKUS is an air compressor that helps move air in and out of your blood pump, helping it fill and eject. Your Berlin Heart makes a humming sound, which is normal. A computer sits on top of the IKUS and allows doctors to adjust the settings of your Berlin Heart. There are several settings your care team may adjust, like the air pressure strength, how often the air pressure moves in and out, and how many times your Berlin Heart pumps.
Benefits

The Berlin Heart helps patients with heart failure, as it improves blood circulation. A Berlin Heart may help reduce heart failure symptoms and improve quality of life while waiting for a heart transplant or your heart to get better.
Risks
 There are some risks with a Berlin Heart, but your care team will work hard to keep you safe.
There are some risks with a Berlin Heart, but your care team will work hard to keep you safe.
Infection
The soft cannula will come out of your lower chest and will need to be cleaned frequently. This is important because bacteria lives on your skin and may cause an infection at your cannula site. You may feel nervous the first few times your dressings are changed, but your care team will be there to support you.
Stroke
There is a risk of stroke with all VADs. A clot can form in the VAD, become dislodged, and may travel up a blood vessel to the brain. A blood clot in the brain leads to a decreased blood flow to the brain in that specific area, and this is called a stroke. Your care team will manage your blood thinner medicines and levels carefully to try to prevent a stroke. Sometimes, even with perfect levels, a stroke will occur.
Your care team will monitor you for the following symptoms:
- Headache
- Confusion
- Numbness and/or tingling on one side of the body
- Weakness on one side of the body
- Slurred speech
Bleeding
There is a risk of bleeding with all VADs. To prevent clots from forming in the device, you have to be on a blood thinner. Sometimes the blood thinner will lead to bleeding that may require a change in medicines, a blood transfusion, or in some cases, a surgery to stop the bleeding. Your care team will manage your blood thinner medicine and levels carefully to try to prevent bleeding. Sometimes, even with perfect levels bleeding will occur.
Pediatric VAD Infections
Download the pdf to learn more.
Take ACTION Reducing Stroke Rates
Download the pdf to learn more.