Understanding
Your Diagnosis
Heart failure is a complicated condition and can affect people of all ages. Learn the basics about heart failure and explore the different types symptoms, risk factors, and complications.
Heart failure is a complicated condition and can affect people of all ages.
Learn the basics about heart failure and explore the different types,
symptoms, risk factors, and complications.
1
Overview
2
Causes
3
Testing
What is Heart Failure?
The heart is one of the most important parts of your body. But what happens when it doesn’t work like it should? This video explores what heart failure is and some of the causes.
Read through our Heart Failure Success Patient and Family Education Handbook, check out An Introduction to Pediatric Heart Failure and watch the animated video below to better understand heart failure.

Download

Heart Failure
Download

Normal Heart Structure
and Function
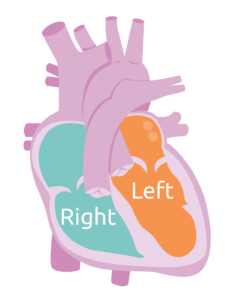
A normal heart has 4 chambers: 2 atria and 2 ventricles. The right side of the heart receives deoxygenated (blue) blood from the body and pumps it to the lungs to get oxygen. The left side of the heart receives the newly oxygenated blood (red) from the lungs and pumps it to the rest of the body.
The heart has two phases: contraction (systole) and relaxation (diastole). When the heart relaxes, the ventricles rest and fill up with blood sent from the atria. During contraction, the ventricles squeeze the blood to the rest of the body.
What are the Different Types of Heart Failure?
Heart failure can be classified based on whether the ventricle has abnormal contraction or abnormal relaxation.
Systolic Heart Failure
If the ventricle can’t contract well enough to pump blood to all parts of the body (including your brain, muscles, and other important organs), we call it systolic heart failure. Systolic heart failure can cause you to feel unwell and weak. It can also cause your other organs to not work properly.
Diastolic Heart Failure
If the ventricle can’t relax well enough to fill properly, we call it diastolic heart failure. This can happen if your heart muscle becomes stiff or thick. Diastolic heart failure can lead to blood backing up into the lungs and cause shortness of breath. When diastolic failure is severe, your heart cannot fill up with enough blood to adequately supply your body and your important organs. Sometimes you can have both systolic and diastolic heart failure.
Heart failure can also involve the left ventricle (left-sided heart failure), right ventricle (right-sided heart failure), or both (biventricular).
Left-sided Heart Failure
The left ventricle is the heart’s primary pumping chamber. With left-sided systolic failure, the left ventricle struggles to pump enough blood throughout the body. This can lead to blood building up in your lungs. As the blood backs up into your lungs, it can make it hard for you to breathe and cause you to cough, especially if you’re doing activities like exercising or playing.
Right-sided Heart Failure
Right-sided heart failure often happens as a result of left-sided heart failure. With right-sided heart failure, the right ventricle loses some of its pumping power. In other words, it becomes too weak to pump enough blood to your lungs. When the right ventricle struggles to pump, blood builds up in your liver and veins. This can cause swelling in your legs, abdomen (belly), and feet.
Biventricular Heart Failure
Biventricular heart failure is when both sides of your heart are affected. Your symptoms can be a combination of left- and right-sided failure.
Symptoms
Complications
Symptoms

Living with heart failure can be challenging. What does it feel like when your heart doesn’t work like it should?
Life with heart failure looks different for each patient and depends on your age. Your symptoms will depend on how severe your condition is and how much of your heart is affected. Some common symptoms of heart failure include:
- Shortness of breath, especially with physical activity
- Rapid breathing
- Chronic cough and congestion in your chest
- Swelling in your legs, face, and sometimes abdomen
- Excessive sweating
- Rapid heart rate or palpitations
- Feeling like you need to take breaks while playing or exercising
- Fatigue (tiredness)
- Nausea or vomiting
- Belly pain
- Loss of appetite
- Not able to lie flat when sleeping or waking up gasping for air
- Skin changes: cold and clammy, or sweaty, flushed, and warm to the touch
- For infants, trouble feeding, difficulty gaining weight, falling asleep while eating, sweating while eating, and rapid breathing are most common.
Complications

Depending on your age and the cause of your heart failure, it’s possible that you may face some complications.
- Poor growth: For many different reasons, heart failure can make it hard for you to grow as you would if your heart were working normally.
- Arrhythmias: In some cases, heart failure can lead to abnormal heart rates or rhythms. Cardiac arrhythmias mean your heart’s electrical impulses aren’t working correctly. Serious arrhythmias can be life threatening and sometimes require medications and/or an internal defibrillator.
- Heart valve issues: Heart failure can stretch out your heart. When this happens, your heart valves may not close properly. This causes them to become leaky, which causes some blood to move backward. Leaky valves can worsen heart failure.
- Kidney insufficiency and/or failure: Heart failure can limit the blood flow to your kidneys. Over time, this takes a toll and can lead to kidney failure.
- Liver disease: If your heart failure leads to fluid retention, this can cause pressure and scarring in your liver, making it hard for your liver to work like it should.
- Clots: If your heart does not squeeze out blood properly, clots can form within the heart. These clots can be dangerous if they go to other parts of your body and brain.
 Living with heart failure can be challenging. What does it feel like when your heart doesn’t work like it should?
Living with heart failure can be challenging. What does it feel like when your heart doesn’t work like it should?
Life with heart failure looks different for each patient and depends on your age. Your symptoms will depend on how severe your condition is and how much of your heart is affected. Some common symptoms of heart failure include:
- Shortness of breath, especially with physical activity
- Rapid breathing
- Chronic cough and congestion in your chest
- Swelling in your legs, face, and sometimes abdomen
- Excessive sweating
- Rapid heart rate or palpitations
- Feeling like you need to take breaks while playing or exercising
- Fatigue (tiredness)
- Nausea or vomiting
- Belly pain
- Loss of appetite
- Not able to lie flat when sleeping or waking up gasping for air
- Skin changes: cold and clammy, or sweaty, flushed, and warm to the touch
- For infants, trouble feeding, difficulty gaining weight, falling asleep while eating, sweating while eating, and rapid breathing are most common.
 Depending on your age and the cause of your heart failure, it’s possible that you may face some complications.
Depending on your age and the cause of your heart failure, it’s possible that you may face some complications.
- Poor growth: For many different reasons, heart failure can make it hard for you to grow as you would if your heart were working normally.
- Arrhythmias: In some cases, heart failure can lead to abnormal heart rates or rhythms. Cardiac arrhythmias mean your heart’s electrical impulses aren’t working correctly. Serious arrhythmias can be life threatening and sometimes require medications and/or an internal defibrillator.
- Heart valve issues: Heart failure can stretch out your heart. When this happens, your heart valves may not close properly. This causes them to become leaky, which causes some blood to move backward. Leaky valves can worsen heart failure.
- Kidney insufficiency and/or failure: Heart failure can limit the blood flow to your kidneys. Over time, this takes a toll and can lead to kidney failure.
- Liver disease: If your heart failure leads to fluid retention, this can cause pressure and scarring in your liver, making it hard for your liver to work like it should.
- Clots: If your heart does not squeeze out blood properly, clots can form within the heart. These clots can be dangerous if they go to other parts of your body and brain.
Heart Failure Resources
For more information about pediatric heart failure, see the following resource.
Pediatric Heart Failure: A Guide for Parents and Families
The Children’s Cardiomyopathy Foundation developed a guidebook providing a comprehensive overview of heart failure, including signs and symptoms, diagnostic testing, medications, and advanced heart failure therapies. The resource draws on the experience and knowledge of the top pediatric heart failure specialists in the U.S. and Australia.
Hearts & Minds: Neurodevelopment in Patients with Heart Failure & VADs
Prompted by needs and interests of our Families in ACTION (FACT) Committee, ACTION recently joined forces with a fellow Cardiac Networks United organization, the Cardiac Neurodevelopmental Outcome Collaborative to:
- develop patient and family resources specific to neurodevelopment in pediatric heart failure and VAD patients, and
- better understand current practices among ACTION sites specific to neurodevelopmental care and education.
This cross-network collaboration brought together experts in pediatric psychology, neuropsychology, cardiology, nursing, and more to address this important aspect of care for patients and families.




